Before the Procedure

A patient checks in to the clinic.
When you arrive to the Interventional Pain Clinic you will be checked in at the front desk. A nurse will bring you to the pre-operative suite where a stretcher is waiting for you. Most procedures do not even require a hospital gown, but if needed, we will provide one. The nurse will get you comfortable while your vital signs are taken. If you are diabetic, we will do a finger stick to check your blood sugar. Since many of our procedures contain steroid, we will sometimes cancel/postpone procedures for blood sugar elevations for your safety.
You will also be asked if you take any anticoagulant medications (commonly known as blood thinners). Aspirin, Coumadin, Plavix, Pradaxa, Xarelto, and Eliquis are the most commonly used blood thinners but many commonly used over the counter medications like Fish Oil, Omega -3, garlic, and ibuprofen have anticoagulant properties. Please bring your medication list. For your safety, blood thinners must be held for a certain number of days before the procedure. We will contact your prescribing physician to request clearance to hold the blood thinner for the appropriate number of days. If your physician does not feel it is safe for you to be off your blood thinner, we will re-evaluate you for other options to control your pain.
If you have any questions please refer to the Anticoagulation Guidelines at the end of this page. Remember, do not stop any medications without speaking to your prescribing physician, primary care doctor, or cardiologist.
Sedation
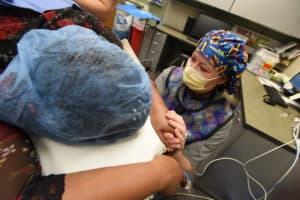
A nurse holds a patient’s hand during a procedure.
Most patients undergo interventional pain procedures without the need for sedation. Our physicians always ensure that proper local anesthetic is used to numb the skin prior to needle insertion. There are also times when sedation should not be given so the patient can report relief of pain or change in the intensity of pain. A few examples of procedures that do not usually require sedation are Epidural Steroid injections, Transforaminal Epidural Steroid Injections, Medial Branch Blocks, and SI joint injections.
Patients with significant anxiety, significant pain, or undergoing procedures that require you to remain motionless for prolonged periods of time may require sedation. Some examples of these procedures are Kyphoplasty, Spinal Cord Stimulator Trials, and Radiofrequency Ablations. In these cases, a small IV is inserted before the procedure and medication is given in the procedure room. The medication will help you relax and control your anxiety. All of our physicians are licensed anesthesiologists and a nurse will monitor your breathing, oxygen levels, and blood pressure during and after the procedure. Patients receiving sedation will be monitored for at least 30 minutes after the procedure.
There are a few rules for receiving sedation:
NPO Guidelines
- No heavy food or dairy products for eight hours before your procedure.
- You may have light food like toast or bread up to six hours before your procedure.
- You may have clear liquids like black coffee, tea, Sprite, water, or Gatorade until two hours before your appointment.
Responsible Adult
- There must be a responsible adult in the clinic during the procedure visit that can drive you home. One question that is frequently asked is “can I ride public transportation since I won’t be driving?” The answer is “Yes, you may, as long as there is someone riding with you.” The driver can’t be responsible for someone who has been sedated.
During the Procedure
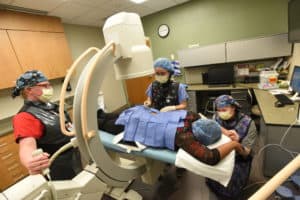
Patient in a procedure room
You will be taken to the procedure on the stretcher and asked to roll over onto the procedure table. The staff will help you get in the correct position then the nurse will place a blood pressure cuff on your arm, wires on your chest to monitor your heart rate and rhythm, and a probe on your finger to monitor your oxygen.
If you are receiving sedation, it will be given after your first set of vital signs are taken.
The skin around the injection site will be thoroughly washed with an antiseptic soap to help prevent infection. After it dries, the doctor will inject numbing medicine under your skin. This does sting, but will go numb after a few seconds.
We use x-ray, called fluoroscopy, or ultrasound guidance with almost all of the procedures. This allows the physician to know the location of the needle tip at all times for your safety.
After the Procedure

Nurses with a patient after a procedure
The stretcher will be brought into the procedure room and the staff will help you roll back onto it. You will be taken to the recovery area where another set of vital signs will be taken. If you did not receive sedation, the discharge nurse will go over the post procedure instructions and you will be discharged.
If you were sedated, your vital signs will continue to be monitored during your recovery time. We have juice and crackers if you want a snack. When you have recovered from the sedation, and your vital signs are stable, your IV will be removed and the nurse will give you the post procedure instructions before you are discharged.
Remember to check out at the front desk on your way out and if a follow up appointment needs to be scheduled, it can be done before you leave.
As always, we welcome your questions and comments, so don’t hesitate to call us at 501-686-8818.